 
Many simulation, animal and observational studies have been performed on all manner of aspects of CPR, including compression depth, recoil, and speed. Below, we’ll review some of the key concepts of high-quality CPR. 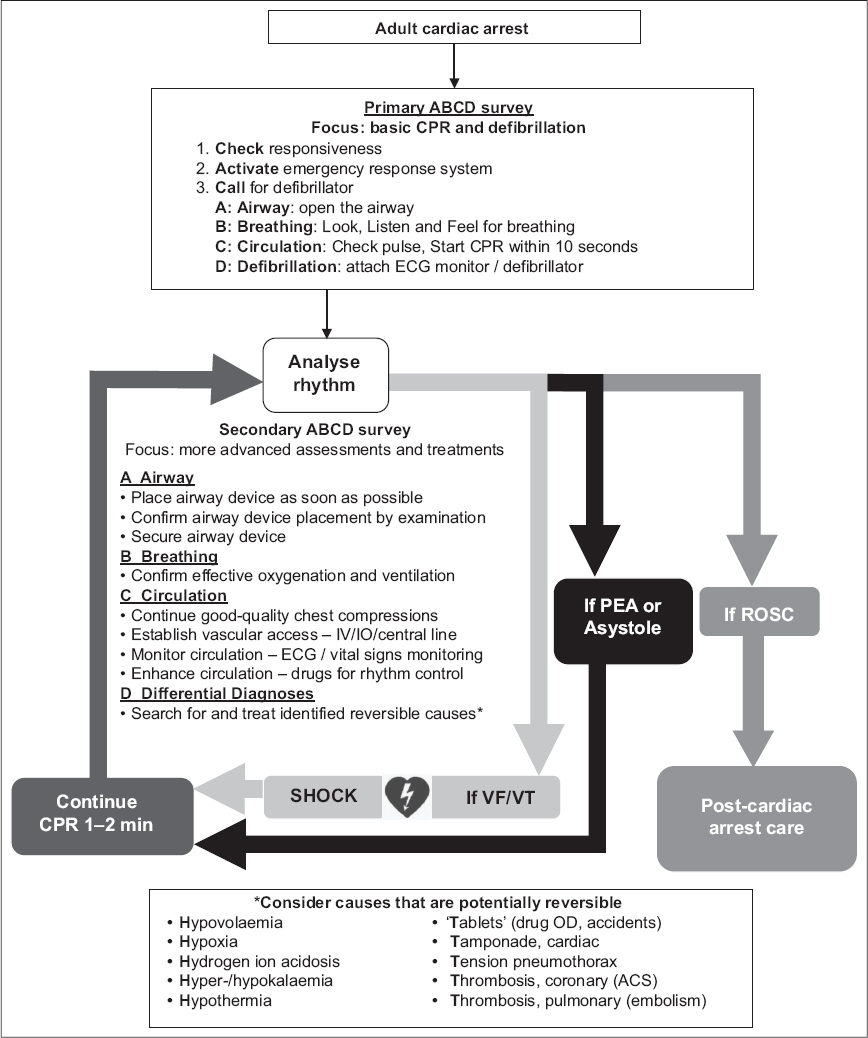
In other words, the theory is that you can run a code in the field, in the ER, or in the back of an ambulance, but the sooner you run it well, the better odds a patient has of a good outcome. Although there are a myriad of factors that play into treating OHCA patients – airway use, mechanical or manual CPR, ACLS drugs, etc., the idea behind emphasizing on-scene CPR is that it gives EMS agencies the opportunity to defibrillate as soon as possible, perform great CPR and increase a patient’s chance of ROSC by re-establishing myocardial perfusion, instead of focusing on patient packaging and transport. Historically, we know that certain factors in OHCA have prognostic importance and are associated with better outcomes, including witnessed arrest, time to CPR and defibrillation, initial shockable rhythm (VT/VF), AED use, and patient ageiii. Clearly, OHCA is an important topic and is worth exerting considerable effort to improve outcomes. Extrapolating these statistics to Rhode Island’s population of 1 million, we can estimate that approximately 1100 Rhode Islanders are having OHCA each year, or 3 people every day. 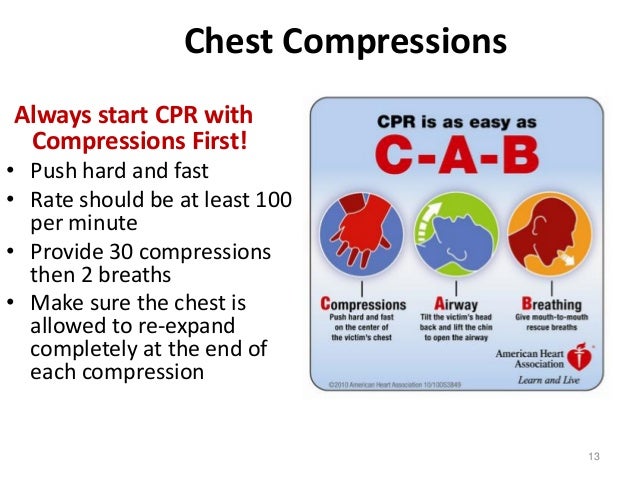
Studies vary, but the overall survival rate for OHCA is anywhere from 6-12%, nationally. According to the American Heart Association (AHA), approximately 355,000 people each year suffer an OHCA event (110 events per 100,000 population). Traditionally, EMS providers have also been taught to transport OHCA patients to hospitals quickly as well, so asking them to remain on-scene for up to 30-minutes is controversial. When treating trauma patients, for example, EMS providers are instructed to transport as quickly as possible to a hospital. Pre-hospital medicine policies and protocols vary according to the region, state, resources, distance from definitive care, and culture. In March of 2017, the Rhode Island Department of Health instituted new protocols requiring EMS providers to stay on the scene of an atraumatic cardiac arrest for up to 30-minutes, or until return of spontaneous circulation (ROSC) is achieved. In this article, we’ll discuss CPR, Rhode Island State EMS protocols, and the evidence for and against them. Fortunately, there have been a number of trials conducted that can inform our practice, and large, curated resuscitation outcomes databases exist for retrospective studies. Firstly, there have been a very limited number of prospective, randomized and controlled trials on CPR and resuscitation due to many inherent barriers to performing such a study – cost, the infrequency of out-of-hospital cardiac arrest (OHCA), and the difficulty and ethical concerns inherent in studying something which is thought to be efficacious (CPR) against something else which may not be. When discussing CPR and the holy grail of evidence-based practice, there are a number of caveats to acknowledge. The latest iteration of CPR and resuscitation science is the focus on “high quality” CPR, “team-focused” CPR and “cardiocerebral resuscitation” (CCR). In the mid 2000s, external CPR devices became more common and in 2010 “hands-only” CPR was the predominant layperson resuscitation method. In the 1990s, pubic defibrillators became mainstream. Since then, CPR has gone through a number of changes, from compression-to-ventilation rates, training programs and even the manner in which it is delivered. CPR as we know it was “invented” by numerous resuscitation scientists working in competing labs during the 1950s.
0 Comments
Leave a Reply. |
Details
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
